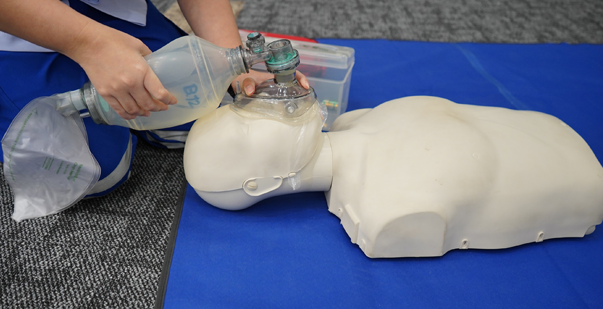
A bag-valve mask (BVM) is a self-inflating bag offering ventilation to a person not breathing normally. A BVM comprises a non-rebreathing valve and a face mask. The opposite end of the bag attaches to the source of the oxygen. Hold the mask against the face. Then squeeze the bag to offer ventilation to the patient through the mouth and the nose until intubation is complete. Read the blog to explore more about BVM ventilation, and its techniques.
What is bag-valve mask ventilation?
BVM ventilation is a crucial skill for emergency providers. This technique helps to restore breathing in patients who are not spontaneously breathing. A BVM is an emergency procedure that is performed until intubation.
Factors that cause difficulty in BVM ventilation include the following:
- BMI greater than 26
- Lack of teeth
- Presence of facial hair
- History of snoring
- Age above 55 years
What are the criteria for BVM ventilation?
Here are the criteria for BVM ventilation:
- An open airway
- Proper ventilation technique
- Properly sealed masks
- Valve for proper oxygenation
How to master BVM ventilation?
So ‘what is the most effective way to deliver bag-mask ventilation?’ Mastering BVM ventilation is, although considered a basic procedure, there is nothing ‘basic’ about it. It requires extensive experience and training. Although it is a vital part of airway management, most people do not know the right techniques. It is a challenging skill requiring practice and experience.
When it is performed in an emergency, it can lead to respiratory failure or cardiac arrest. The mask is placed on the faces of the patients while administering ventilation aggressively. When this is not recognized, the airway gets bloodied with gastric contents during intubation. This makes it all the more challenging. As a result, hypoxia worsens and aspirin occurs, leaving the patient at risk of experiencing cardiac arrest.
What is the equipment for BVM ventilation?
- Beg-valve apparatus
- Gloves, mask, gown, and eye protection
- Pulse oximeter
- Nasogastric tube
- Oxygen source
- Capnography equipment
- Suctioning apparatus and Yankauer catheter
Read More: Elements of Effective Team Dynamics in ACLS
How do you know when ventilation is effective?
Clinical detection of adequate ventilation is challenging. The traditional CE method is not the best technique. Here are a few factors that contribute to poor BTM ventilation:.
- Poor mask seal: While using the traditional CE technique, uneven pressure is often common. This means that while using the left hand, there is a probability for the air to leak between the mask and the right side of the patient’s mouth. This is often recognized.
- Improper positioning: Due to the inherent difficulty in maintaining a quality seal, there is a strong tendency to push the mask onto the face. The mouth is closed, which makes the nares the only route of ventilation. This leads to the obstructive soft tissues of the pharynx being collapsed, which blocks the glottic opening. This two-handed technique is sometimes called thenar eminence (TE).
- Excessive rate and tidal volume (hyperventilation): There can be a significant difference between what you are doing and what you are actually doing. In the Milwaukee study, paramedics were taught to ventilate at the appropriate rate during cardiac arrest. They looked at the ventilation rates objectively, and the average rate was 30 breaths per minute. Excessive tidal volume and excessive rate increase the likelihood of exceeding the pressure of the lower esophageal sphincter. This helps deliver large tidal volumes of air to the stomach.
How are breaths delivered using a bag-mask device?
So ‘how are breaths delivered using a bag mask?’ Open the airway to prevent gastric inflation and deliver breaths slowly. When your own heart rate goes to 150 beats per minute, it can be difficult to wait for 6 seconds to deliver a breath. If the patient is intubated, you can place them on the ventilator. Purchase a timing light that goes on the end of the BVM.
While delivering breaths too fast, you might often deliver too much. However, make sure that the volume of air during BVM is 1600 millimeters. It is not necessary to squeeze the bag until the opposite sides of the BVM touch. Compress only 1/3 of the bag to give a large enough tidal volume.
What is the correct volume of air during BVM?
An adult BVM with oxygen supplied at a minimum of 16 liters per minute can deliver up to 1.5 liters of oxygen per breath.
Read More: ACLS certification: What is it, and who needs it?
BVM ventilation during cardiac arrest
If you are doing 30:2 during BLS CPR, you must not take your breaths slowly. Instead, you must resume compressions within 3 seconds. To do so, it will take 5 to 6 seconds to breathe and cannot be given quickly.
Prioritize ‘little bag squeeze, little bag squeeze’ while prioritizing full releases between squeezes. Elevate intrathoracic pressure without a full release, and the increased intrathoracic pressure impedes venous return.
Warning for BVM ventilation
Do not place your hands or mask over the patient’s eyes. This may damage the eyes, causing a reaction.
Conclusion
Thus, to master BVM ventilation, adopt the ‘two thumbs down’ technique and deliver breaths slowly. Compress 1/3 of the bag and give breaths quickly during cardiac arrest, allowing full release of BVM.